PITT-Inflame (ERC)

2026-01-22
Würzburg Researchers Discover a Novel Inflammatory Function of Platelets
„PITTs“ redefine platelet biology – study published in Science

Würzburg. Platelets are small, anucleate blood cells that play an essential role in hemostasis. Their primary task is to recognize vascular injury, become activated, and aggregate via their surface receptor integrin αIIbβ3. This leads to the formation of a stable platelet plug that seals the wound and stops bleeding. When this process becomes dysregulated, however, it can result in vessel-occluding clots – so-called thromboses – which may cause myocardial infarction or stroke.
A surprising platelet mechanism beyond classical activation
The classical role of platelets in hemostasis and thrombosis has been well understood for decades. However, a team from the Institute of Experimental Biomedicine at the University Hospital Würzburg (UKW) and the Rudolf Virchow Center (RVZ) of Julius-Maximilians-Universität Würzburg (JMU) has now uncovered a surprising cellular mechanism, published in Science, that fundamentally changes our view of platelet biology. During severe pathological conditions such as infections or infarction, platelets can switch to a completely different functional program. In this context, integrin αIIbβ3 serves as a building block of a novel organelle that is released by platelets and drives damaging inflammatory processes.
The researchers observed that under such conditions, platelets form and shed tiny, filamentous membrane extensions—so-called PITTs. PITT stands for Platelet-derived Integrin- and Tetraspanin-rich Tethers and refers to integrin- and tetraspanin-enriched membrane structures released from platelets. These PITTs bind to immune cells and the vessel wall and activate them, while the detaching platelets themselves remain weakened and less adhesive in the bloodstream.
Professor Bernhard Nieswandt, senior author of the study and Chair of Experimental Biomedicine I at UKW, explains:
“Normally, platelets become activated only upon vascular injury. They change shape, release signaling molecules, and form a thrombus. With PITTs, the opposite happens: platelets do not undergo classical activation. Instead, they shed comet-tail-like organelles from their membrane network that are rich in αIIbβ3 and the tetraspanin co-receptor CD9, while other surface molecules remain on the platelet. This is a completely novel mechanism that has not been observed in any other cell type and raises fundamental questions about membrane organization and regulated protein mobility.”
From patient blood samples to mouse models
PITT formation was first discovered in blood samples from patients with severe sepsis, serious bacterial infections, and COVID-19. The researchers detected the filamentous tethers in blood smears and simultaneously observed a loss of αIIbβ3 from the platelet surface. Further studies in animal models and using intravital microscopy demonstrated that PITTs form directly within blood vessels during inflammation or infection and attach to immune cells and the vessel wall. This leads to activation of these cells and amplification of vascular inflammation.
“That platelets redistribute αIIbβ3 in this way and thereby lose their normal clotting function was completely unexpected,” emphasizes Professor David Stegner, group leader at the RVZ and co-first author of the study alongside Charly Kusch. “This may explain why many critically ill patients suffer simultaneously from tissue-damaging inflammation and an increased risk of bleeding.”
New therapeutic perspectives
The researchers further showed that blocking αIIbβ3 with monoclonal antibodies significantly reduced PITT formation and, consequently, severe inflammatory responses and tissue damage in disease models. This opens new therapeutic avenues to specifically target so-called thrombo-inflammatory disease mechanisms without impairing vital hemostasis.
Funding and international collaboration
The study was conducted within the framework of the Collaborative Research Center (SFB) 1525 “Cardio-Immune Interfaces,” funded by the German Research Foundation (DFG), and was additionally supported by the ERC Advanced Grant “PITT-Inflame” from the European Union.
In addition to several Würzburg-based research groups, collaborators from France, Italy, and the United States were involved.
Figure
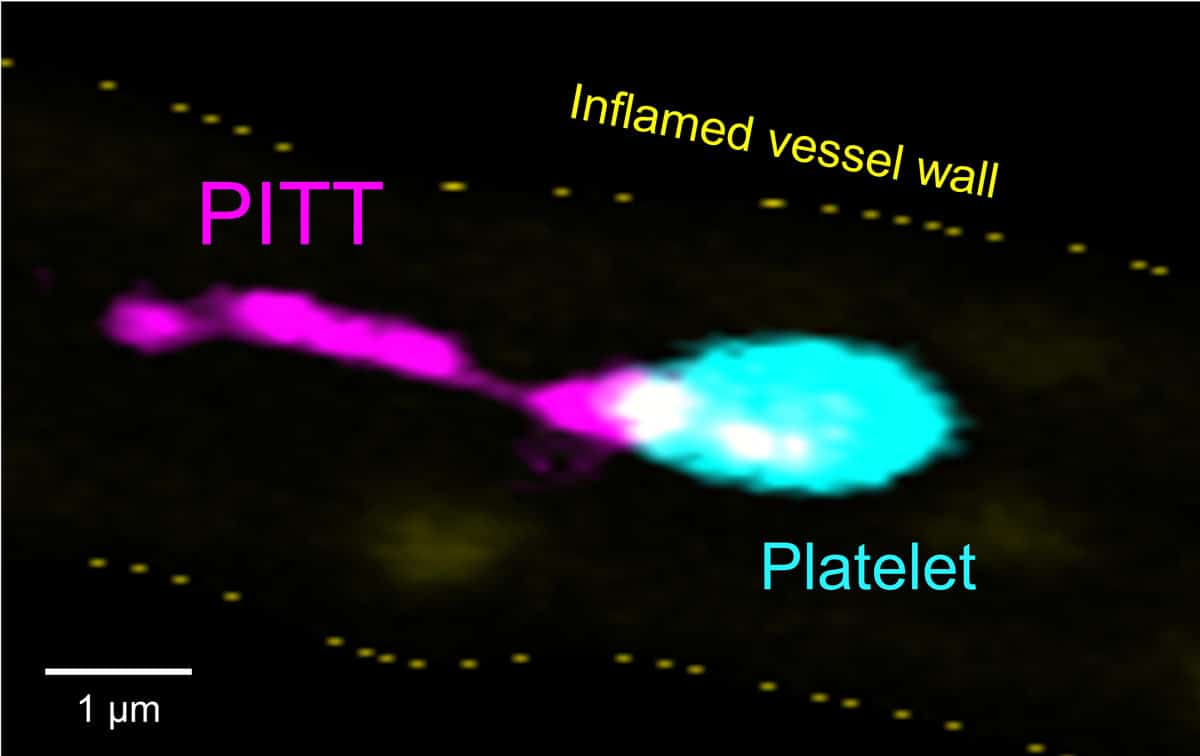
A single platelet forming pro-inflammatory PITTs in an inflamed blood vessel.
Intravital microscopy image from the liver of a mouse model: a platelet (turquoise) adheres to the inflamed vessel wall (yellow dashed outline) and sheds a long, filamentous membrane extension—a so-called PITT (magenta). These platelet-derived integrin- and tetraspanin-rich tethers remain deposited at the vessel wall and promote inflammatory responses, while the platelet itself re-enters the bloodstream. Scale bar: 1 μm.
Publication
Kusch C.*, Stegner D.*, Weiß L.J., Nurden P., Burkard P., Johnson D., Bergmeier W., Onursal C., Navarro S., Hackenbroch C., Pfeiffer D., Bonfiglio S.I., Meub M., Groß C., Schenk J., Fumagalli V., Mott K., Bender M., Iannacone M., Andres O., Kastenmüller W., Heinze K.G., Sauer S., Schulze H., Ley K., Nurden A.T. & Nieswandt B. “Platelet-derived integrin- and tetraspanin-enriched tethers exacerbate severe inflammation.” Science 391, eadu2825 (2026). DOI: 10.1126/science.adu2825.
Contacts
Prof. Dr. Bernhard Nieswandt & Prof. Dr. David Stegner
Institute of Experimental Biomedicine – Chair I, University Hospital Würzburg & Rudolf Virchow Center for Integrative and Translational Bioimaging, University of Würzburg
ERC Advanced Grant: 2.5 Million Euros for Bernhard Nieswandt

Professor Bernhard Nieswandt is investigating a cellular mechanism in blood platelets that appears to play a crucial role in inflammatory diseases. He has been awarded an ERC Advanced Grant for his work.
Platelets: Helping in coagulation and driving inflammation
Prof. Dr. Bernhard Nieswandt has been awarded a prestigious ERC Advanced Grant worth 2.5 million euros by the European Research Council for his research on a cellular mechanism in blood platelets that appears to play a crucial role in inflammatory diseases.
Würzburg (04/11/2024): In the mid-19th century, they were first observed as small spheres in the blood, and by the turn of the century, their function in blood clotting, known as haemostasis, and the development of thrombosis were discovered. A few years later, the site of their formation in the bone marrow was also identified, where platelets are shed from their giant precursor cells, the megakaryocytes. The biology of these small, nucleus-free cells, which are only one-thousandth of a millimetre in size and of which we have about 250 million in every millilitre of blood, has gradually evolved into a major research area. It has become obvious that platelets have a plethora of functions beyond stopping bleeding or triggering heart attacks. As modulators of the immune system, they also drive inflammatory processes and thereby promote tissue damage in many disease settings.
Thrombo-Inflammation: Inflammatory Processes Triggered by Platelets
Prof. Dr. Bernhard Nieswandt, Head of the Department of Experimental Biomedicine I at the University Hospital Würzburg and Research Group Leader at the Rudolf Virchow Center, has made seminal contributions to these discoveries and coined the term “thrombo-inflammation.” For his pioneering work in platelet research, his latest discovery, and further investigations, he has now been awarded an ERC Advanced Grant of 2.5 million euros. The Advanced Grants of the European Research Council (ERC) are part of the EU programme Horizon Europe and target established leading researchers. The grant is one of the most prestigious and competitive scientific awards and research funding instruments of the EU.
PITT-Inflame: Shed Organelles Steering Immune Functions
The award is both recognition and encouragement for Bernhard Nieswandt to keep on trusting his scientific instincts, conducting research at the forefront, and making breakthroughs in the understanding of diseases such as stroke, sepsis, or acute respiratory distress syndrome (ARDS). Platelets play a crucial role in the development of these diseases. And this is also the focus of the new ERC project “PITT-Inflame,” an acronym for “Platelet-derived Integrin- and Tetraspanin-enriched Tethers as key effectors in thrombo-Inflammation”. PITTs are comet tail-like organelles shed by platelets that interact with other cells in the vascular system, modulate their function and thereby fuel inflammation and tissue damage.
“We want to analyse a cellular mechanism of platelets that has not been described before and which we discovered rather incidentally in my research group,” says Bernhard Nieswandt. “Normally, the life of a platelet ends quickly after its activation and adhesion to injury sites, and it is then removed by phagocytes. However, we observed that non-activated platelets undergo an unexpected process of cellular reorganization in the bloodstream, allowing them to deposit parts of their membrane at sites where inflammatory processes occur, thus fueling them.” In the first part of the ERC project, Bernhard Nieswandt aims to explore the mechanism of this reorganization which makes the platelet shed a small part of its cell body, an organelle filled with communication molecules that control immune functions but also promote inflammatory tissue damage.
100,000 molecules are reorganized
Intriguingly, integrins, specific adhesion receptors connected to the cell’s cytoskeleton, can move freely in the membrane and rapidly relocate 100,000 molecules to a specific region of the cell surface (microdomain). “There must be a kind of sorting machine in the cell that reorganizes the entire pool of its most important adhesion receptors along with associated membrane proteins, the tetraspanins, as building blocks for novel cell organelles, the PITTs,” says Nieswandt. His research has yielded initial evidence that these organelles are loaded with signalling molecules, ribosomes, and RNA, enabling them to alter the function of their target cells. Having reconstructed the detailed molecular composition and architecture of PITTs and deciphering the underlying signalling networks, Nieswandt in the second part of the project aims to identify PITT-induced effects on target cells and deduce therapeutic strategies from the findings.
“With Covid-19, we have fully learned what thrombo-inflammation actually means”
Many of his findings and patents have already been applied successfully in clinical settings or are on their way there. A good example is ischaemic stroke: Even if a thrombus blocking blood supply to a certain part of the brain is successfully removed, and blood flow is restored, an inflammatory reaction promoting brain damage is still seen in the majority of patients. Bernhard Nieswandt and his team uncovered the mechanisms underlying this inflammatory pathology, driven by platelets, together with colleagues of the Neurology Department of the University Hospital Würzburg. Initial preclinical and clinical studies with inhibitors that suppress this inflammatory reaction showed promising results. Also in acute respiratory distress syndrome, which has affected many people, especially in the COVID-19 pandemic, an excessive immune reaction driven by platelets getting out of control is involved. “With Covid-19, we have fully appreciated what thrombo-inflammation actually means,” explains Bernhard Nieswandt. With the glycoprotein VI (GPVI) expressed on the surface of platelets, his research group has identified a promising target for treating such inflammatory disease processes. “By selectively inhibiting GPVI with an antibody, we can prevent the devastating influx of inflammatory cells into lung tissue and significantly reduce the resulting tissue damage in the inflamed lungs, without increasing the risk of inflammatory bleeding,” explains Nieswandt. He has not only discovered a mechanism for inhibiting GPVI but also demonstrated how this receptor can be removed from platelets, which could be of considerable therapeutic benefit in the future.
New avenues for treating a wide range of diseases
Back to PITT-Inflame: “Our hypothesis is that circulating platelets have the capacity to use their principal adhesion and signalling machineries in two fundamentally different ways and thereby switch between the haemostatic and thrombo-inflammatory functions. If proven correct, this would implicate a radically new paradigm in platelet biology, and open new avenues for the treatment of a wide range of diseases with major societal impact,” summarizes Bernhard Nieswandt.
About Bernhard Nieswandt
Bernhard Nieswandt (born in 1968) studied Biology and Biochemistry in Regensburg and Canterbury (UK). As a doctoral student in Regensburg, the focus of his studies was already on platelets and inflammation, an entirely new research field at this time, and developed the world’s first antibodies against mouse platelet receptors, which became important tools in the study of these cells. After completing his PhD in 1997, he moved to the University of Witten/Herdecke, where he completed his habilitation in experimental medicine. In February 2002, he moved to Würzburg, where he has been advancing cardiovascular and neurovascular research with groundbreaking discoveries ever since. He was the first to establish a research group in the newly founded Rudolf Virchow Center, University of Würzburg, became a professor two years later, and was appointed head of the Chair of Experimental Biomedicine I in 2008. With his team, he has laid the foundation for two medications: a Factor XIIa inhibitor from CSL Behring, which has just been approved by the US Food and Drug Administration FDA and is being evaluated by the European Medicines Agency EMA, and GPVI inhibitors, which have just entered clinical phase III studies.
Bernhard Nieswandt has supervised 26 postdocs, 41 doctoral theses, and 24 master’s students in Würzburg so far. Since 1999, he has published over 320 papers, cited more than 26,000 times. Eight patents have been granted, with three more under review. Bernhard Nieswandt lives with his family in Eibelstadt, where he manufactures antibodies for cardiovascular research with his company EMFRET Analytics.
About the ERC Advanced Grants
The ERC Advanced Grants are part of the EU programme Horizon Europe and aim to support groundbreaking research by established leading researchers. The awards are among the most prestigious and competitive in the EU. On Thursday, April 11, the ERC announced the names of a total of 255 outstanding scientists in Europe who will be awarded the ERC Advanced Grant. With the new grants totaling €652 million, research projects in a wide spectrum ranging from natural and life sciences to social sciences and humanities are supported. Germany leads among the successful applicants with a total of 50 awards, followed by France with 37 and the United Kingdom with 28. A total of 1829 applications were submitted. The funding not only supports researchers in breaking new scientific ground but also creates around 2,500 jobs across Europe, says Illiana Ivanova, European Commissioner for Innovation, Research, Culture, Education, and Youth.


